Psoriasis
Home » Conditions » Psoriasis
Award winning dermatology service, with over 20 years on experience
Short waiting lists, on some occasions offering same week appointments
Safe environment, in Care Quality Commission approved facilities
PSORIASIS Treatments Include:
Psoriasis Specialist Advice
Psoriasis is an inflammatory skin condition that causes thickening, redness and scaling. It can affect the whole of the skin including the scalp and nails. For some, it can be associated with arthritis. Psoriasis affects around 2% of people in the UK. It can start at any age but mainly occurs in adults under 35 years old, affecting men and women equally. The condition causes red, flaky patches to form on the skin, which are crusty and covered with silvery scales.
Alternative names: Chronic plaque, guttate, nummular/discoid, palmoplantar pustular, pustular, annular pustular, generalized pustular] – psoriasis, seborrhoeic dermatitis, sebopsoriasis.
What causes Psoriasis?
Psoriasis tends to be intermittent in nature and is characterised by remission and ‘flare ups’. Psoriasis appears when the body replaces skin cells more quickly than usual, so the cells that appear on the surface of the skin are not fully mature. This is likely due to a problem with the immune system, but the exact causes of psoriasis remain unknown. Psoriasis can run in families and be brought on by illnesses, stresses or even some medications. Although there is no cure, the condition can be well controlled with medication.
WHAT ARE THE SYMPTOMS/TYPES OF PSORIASIS?
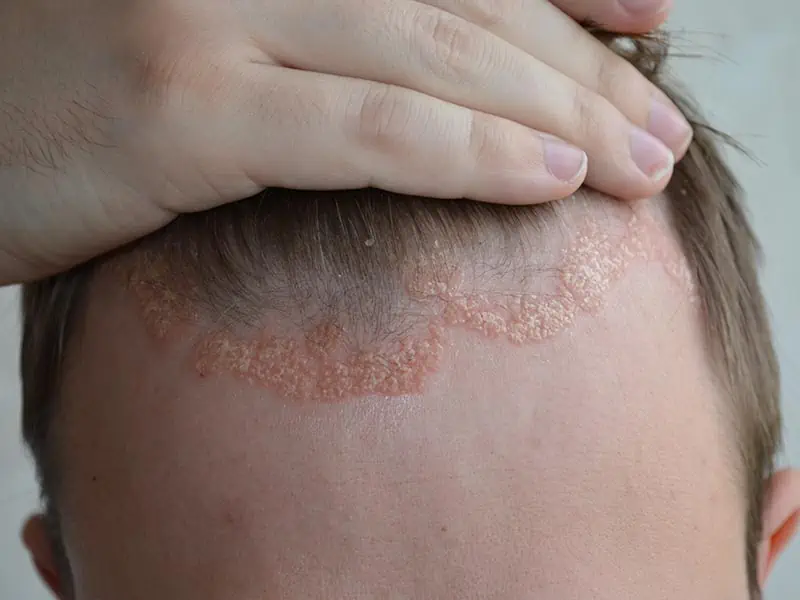
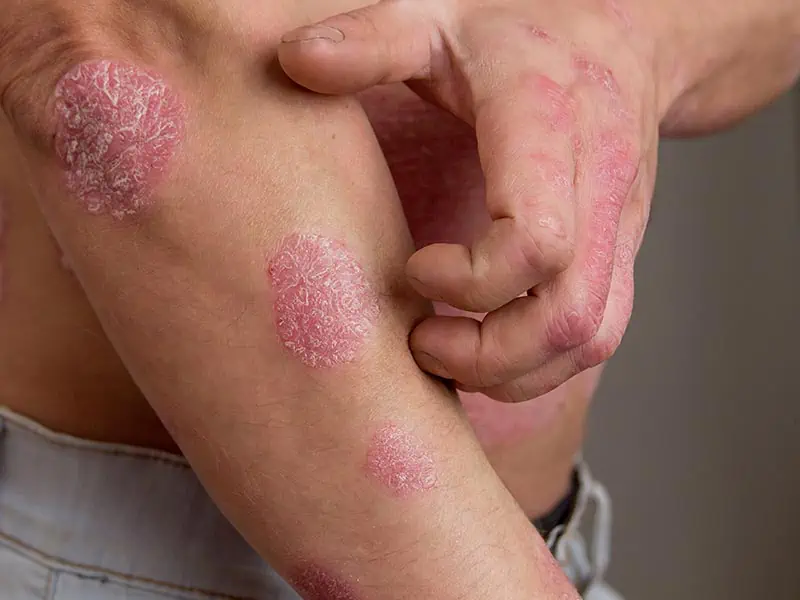
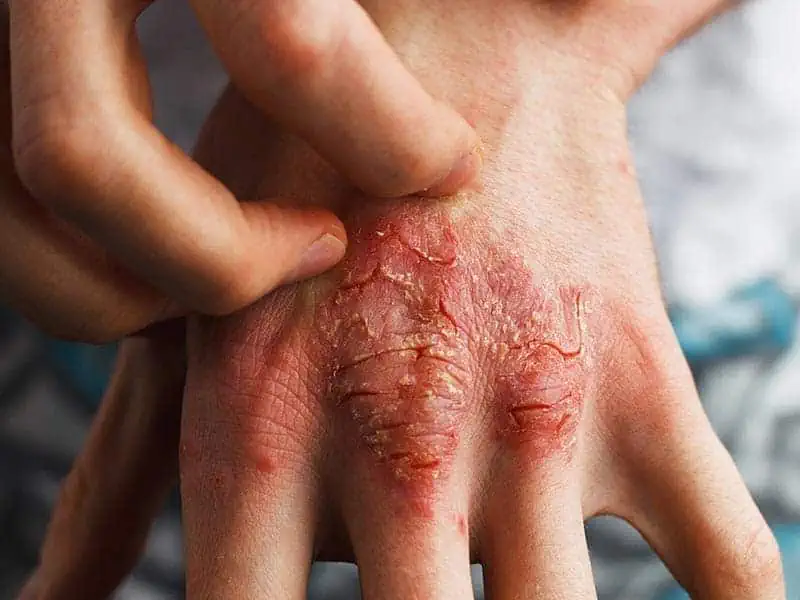
The severity of psoriasis varies a great deal from person to person, with some people experiencing it as a minor irritation, whilst for other people it can have a major impact on their quality of life. Severe psoriasis can cause low self-esteem, as well as the discomfort and pain that can occur with flare-ups of the rash. There are several clinical patterns of psoriasis (see pictures):
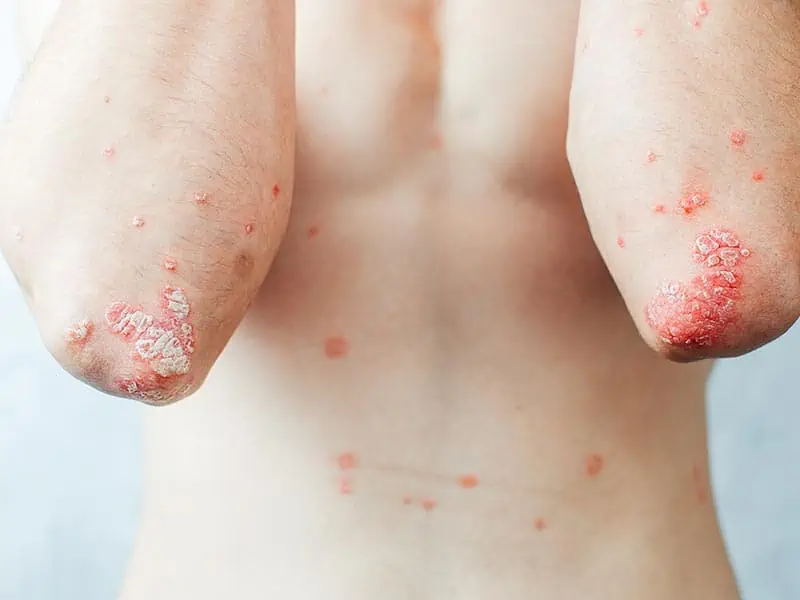
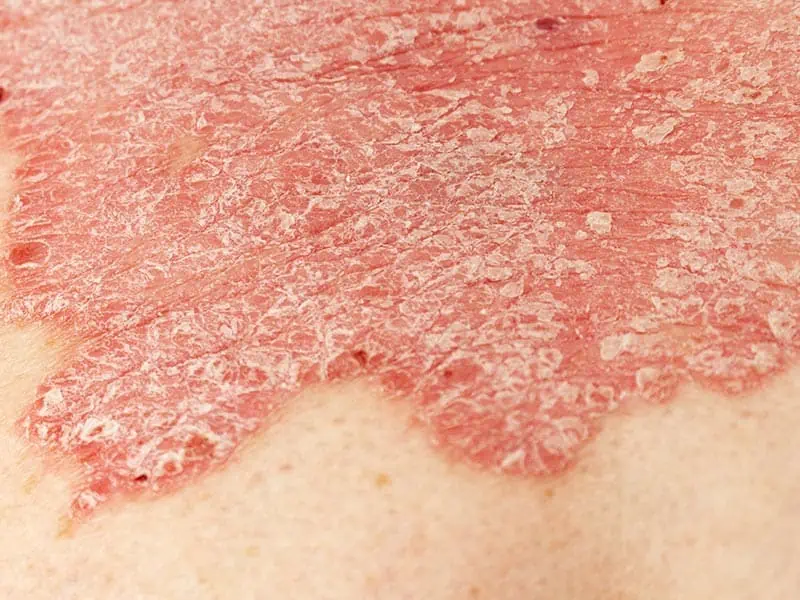
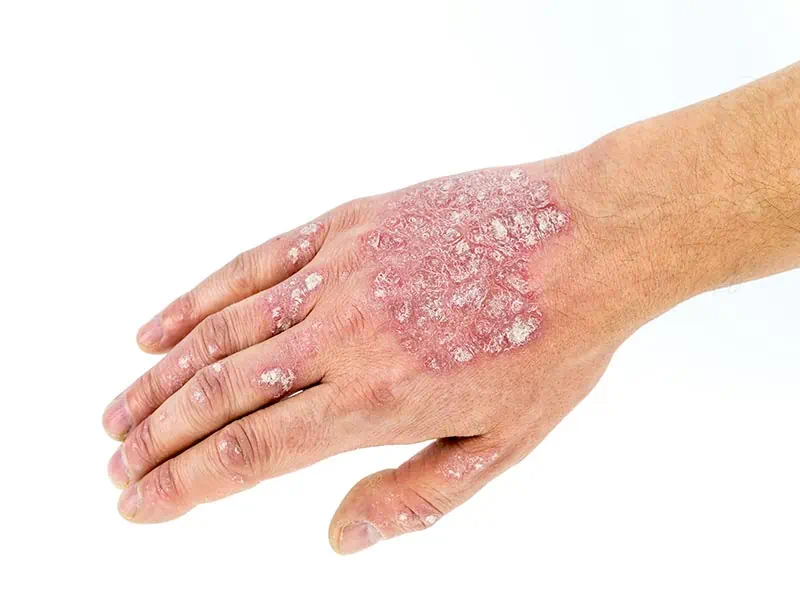
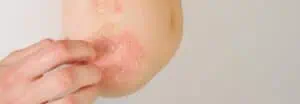
- Chronic Plaque – The most common variant, it tends to occur on the extensor aspects of the elbows and knees and in the scalp. Skin changes include pink or red inflamed, thickened plaques with copious white scale (see image).
- Sebopsoriasis – Similar to scalp psoriasis but can occur on the face, chest, armpits and groin.
- Flexural – Raw, red areas in the groin, armpits or under the breasts.
- Guttate – Multiple small spots of psoriasis that erupt on the trunk following a sore throat or illness (see image).
- Erythrodermic – Extensive disease covering more than 90% of the body surface area.
- Palmoplantar pustular – Pus-filled inflamed spots and the palms and soles.
- Pustular – The most severe form of psoriasis, skin lesions are red, tender and filled with pus spots.
HOW CAN PSORIASIS BE TREATED?
Unfortunately, there is no cure for psoriasis, but there are a number of ways in which you can manage the symptoms and minimise the discomfort that the rash can cause. Our consultant psoriasis specialists can offer you expert treatment with a very good chance of dramatically improving your psoriasis.
Creams include emollients, soap substitutes, vitamin D, tar, steroids.
Phototherapy involves precise doses of ultraviolet light being delivered by a medical UV-machine. Our expert dermatology nurses and physician’s assistant run the phototherapy clinic. Sessions may be 2 or 3 times weekly depending on the type of ultraviolet therapy required.
Systemic medications are reserved for severe or life-limiting psoriasis. (For more information on psoriasis, please see the British Association of Dermatologists website treatment for moderate or severe psoriasis advice leaflet).
FREQUENTLY ASKED QUESTIONS
WHAT IS IT LIKE TO HAVE PSORIASIS?
Psoriasis can vary in severity from no more than a minor irritation to being a major problem – in extreme cases, sometimes requiring hospitalisation. Even a small bit of psoriasis in a delicate area such as the face or genitals can cause immense distress. Occasionally it can be itchy or cause painful splitting or fissuring of the skin. As well as the skin being affected, the nails can become abnormally brittle with flaking and pitting. 5% of patients might develop arthritis associated with psoriasis. Although psoriasis is incurable, it can be well controlled with medication.
WHAT ADVICE CAN YOU GIVE FOR LIVING WITH PSORIASIS?
In addition to receiving specific treatment for psoriasis flare-ups, it’s also important that you self-manage your skin condition in order to minimise and prevent flare-ups from happening. Maintaining good physical and mental health will ensure that your immune system is strong and will lessen the risk of joint pain and fatigue that can be associated with psoriasis. Stress is often a trigger for flare-ups of psoriasis and other skin conditions, so beneficial for your health if you can avoid stress as much as possible.
If you’d like to find out more about how we can help you to manage your psoriasis effectively in the long term, please contact us and we’ll arrange a consultation with one of our dermatology specialists.
IS PSORIASIS GENETIC?
Psoriasis can run in families so if you have a close family member who suffers from the condition then you are more likely to have it too. The exact role genetics play in psoriasis is unclear.
WHAT CAN TRIGGER PSORIASIS?
Common psoriasis triggers include:
- an injury to the skin
- alcohol
- smoking
- stress
- puberty
- menopause
- immune disorders
- certain medications
IS PSORIASIS CONTAGIOUS?
No, psoriasis is not contagious
REQUEST A CALL BACK
Please fill in this form and one of our team will give you a call back to arrange a consultation with one of our expert dermatologists.
HEAR FROM OUR PATIENTS
WHY CONSULT WITH A Psoriasis Specialist AT STRATUM DERMATOLOGY CLINICS?
Severe psoriasis can cause low self-esteem, as well as the discomfort and pain that can occur with flare-ups of the rash. We pride ourselves on our successful and comprehensive range of treatments, which are tailored to you as an individual and will allow you to gain your confidence back and manage your psoriasis symptoms.
We work with leading experts in the field of dermatology to ensure you have the best experience and treatment. Stratum Dermatology Clinics are regulated by the Care Quality Commission, are part of the British Association of Dermatologists and are top rated by patients on Doctify so you can assure safe and effective acne treatment with us.
OXFORD
Stratum Clinics Oxford
Blackberry Clinic
Ground Floor, The Quorum
7600 Oxford Business Park
Alec Issigonis Way
Oxford, OX4 2JZ
WIMBLEDON AND RAYNES PARK
Stratum Clinics Wimbledon & Raynes Park
Raynes Park Health Centre
1 Lambton Road
Wimbledon
SW20 0LW
PSORIASIS INSIGHTS AND ADVICE
All About Psoriasis Awareness Month
Observed every August, Psoriasis Awareness Month is a dedicated period for spreading knowledge about psoriasis – a persistent skin disorder affecting millions globally. The campaign is centred around dispelling misconceptions about psoriasis, promoting early diagnosis and advocating for effective treatment strategies. For persons living with
Isotrex Gel
What is Isotrex Gel? Isotrex gel contains the active ingredient Isotretinoin. It belongs to a group of medicines known as retinoids, which are derivatives of vitamin A. When applied to the skin isotretinoin is thought to loosen the cells on the surface of the skin.