Malignant Melanoma
Home » Conditions » Malignant Melanoma
Award winning dermatology service, with over 20 years on experience
Short waiting lists, on some occasions offering same week appointments
Safe environment, in Care Quality Commission approved facilities
Malignant Melanoma Treatments Include:
Everything you need to know
Malignant Melanoma is a type of skin cancer. There are three main types of skin cancer, basal cell carcinoma (BCC), squamous cell carcinoma (SCC) and melanoma. The first two are both known as non-melanoma skin cancer and are the most common varieties.
Malignant Melanoma is less common, accounting for approximately 3% of all skin cancer cases in the UK, which equates to around 16,000 new cases a year. Although less common, malignant melanomas are very serious as they can grow quickly and spread to other organs in the body so it is vital they are diagnosed and treated early.
WHAT CAUSES MALIGNANT MELANOMA?
Melanoma is a skin cancer that usually starts in the skin and develops when skin cells begin to develop abnormally. It can start in a mole or even in normal looking skin and develops when melanocyte cells, the cells that produce brown pigment and moles, grow and divide at a quicker rate than usual.
As with all skin cancers, exposure to ultraviolet light (UV light) is the common cause. You also have an increased risk to developing malignant melanoma if you have lots of moles or freckles. If you have a pale skin type which is prone to burning or have a family history of the disease you are also more at risk.
WHAT ARE THE SYMPTOMS/TYPES OF MALIGNANT MELANOMA?
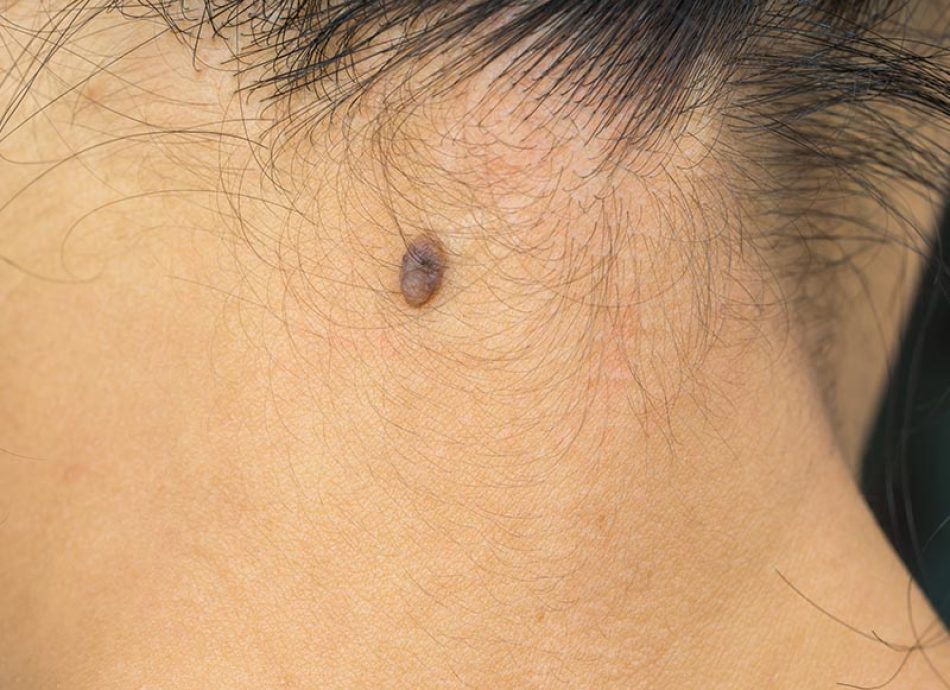
The appearance of a new mole, or any changes to an existing mole could be an indication of a melanoma. This is why it is so important to regularly check and monitor your moles for any changes. In most cases, melanomas are more than one colour and are irregular in shape, they can sometimes be itchy and bleed.
There are four main types of malignant melanoma, superficial spreading melanoma, nodular melanoma, lentigo maligna melanoma, acral lentiginous melanoma.
SUPERFICIAL SPREADING MELANOMA
Superficial spreading melanoma is the most common type of melanoma in the UK. They are more common in people with pale skin. Initially, they will grow outwards, rather than downwards into the skin where they will not pose a problem, however they can grow down deep into the skin where they can spread to other parts of the body.
NODULAR MELANOMA
Nodular melanomas grow much quicker into the deeper layers of the skin so it is vital they are spotted and removed quickly. Their appearance is a changing lump on the skin which is dark in colour and they often ooze or bleed. They often grow on normal skin, rather than an existing mole and commonly appear on the neck, head, chest and back.
LENTIGO MALIGNA MELANOMA
Lentigo maligna melanoma develop slowly over many years in areas which are commonly exposed to the sun such as the face and the arms. As they develop slowly, they are often found in older people, particularly those who have spent a lot of time outdoors. They often look like freckles, but are darker and larger so more noticeable. They will gradually grow bigger and can grow downwards to the deeper layers of the skin forming lumps.
ACRAL LENTIGINOUS
Acral lentiginous melanomas are very rare and appear on the hands or the feet, particularly around a nail. They are most common in people with darker skin but can affect anyone.
HOW CAN MALIGNANT MELANOMA BE PREVENTED?
Melanoma is not always preventable, but avoiding getting sunburned or spending time tanning can increase your risk factor.
Regularly checking and monitoring your moles for changes is vital to spotting malignant melanoma and getting it treated as soon as possible. Here is what you should be looking out for when checking your moles:
A Asymmetry – one half doesn’t match the other half
B Borders – the mole has uneven borders
C Colour – there is a variety of colours in the mole (brown, tan or black)
D Diameter – the mole grows larger than a pencil eraser (¼ inch)
E Evolution – the mole evolves in size, shape, colour, elevation or there is a new characteristic
If you notice any changes to your moles, make an appointment with a consultant dermatologist who will be able to quickly diagnose and if necessary provide treatment.
What malignant melanoma treatments Are Available?
The main treatment for malignant melanoma is surgery to remove the lesion from the skin. If melanoma is diagnosed and treated early enough, surgery is usually successful. Surgical excision works by cutting the cancer away from the skin, ensuring no cancerous cells are left behind. The skin can usually be closed with a few stitches or a skin graft depending the size of the lesion.
Complications can arise if melanoma is not removed as the cells can grow deeper into the layers of the skin. If these cells reach the blood or lymphatic system, they can travel to other parts of the body, meaning it is vital to get your skin assessed by a doctor if you have any concerns before the cancer potentially spreads.
REQUEST A CALL BACK
Please fill in this form and one of our team will give you a call back to arrange a consultation with one of our expert dermatologists.
HEAR FROM OUR PATIENTS
WHY TREAT YOUR SKIN CANCER AT STRATUM DERMATOLOGY CLINICS?
Protecting your skin is, of course, always the best course of action, but if your skin has already been damaged by the sun and presents some changes that you find worrying, make sure you seek professional advice. Our chief clinical director has undertaken and published research on the subject, and it remains one of his specialist areas. The earlier you seek treatment, the more likely you are to have a better result.
If you are looking for a private skin cancer clinic, Stratum Dermatology Clinics have clinics nationwide offering mole checking, mole removal and skin cancer treatment. Here at Stratum Dermatology Clinics, we understand how skin conditions can negatively impact your life. We help hundreds of patients each month and our dermatology experts have a wealth of experience in the assessment, treatment and management of all types of skin cancers.
Working with leading experts in the field of dermatology, we pride ourselves on our successful and comprehensive range of treatments. Stratum Dermatology Clinics are regulated by the Care Quality Commission, are part of the British Association of Dermatologists and are top rated by patients on Doctify. Both Stratum Dermatology Clinics and the consultants who work here are recognised by the main healthcare insurance providers.
FREQUENTLY ASKED QUESTIONS
WHAT DOES MALIGNANT MELANOMA LOOK LIKE?
Melanomas tend to resemble a mole that is undergoing changes in size, shape or colour. They may become lumpy or ‘nodular’ and even ulcerate with bleeding. Sometimes they occur in a pre-existing mole, but around half the time they arise in an area or normal skin.
WHAT SHOULD I BE LOOKING OUR FOR?
- A: Asymmetry – the mole looks unusual, asymmetrical or irregular
- B: Border – the border becomes blurred, ill-defined or irregular
- C: Colour – more than 2 colours appear in the mole including brown, black or light areas giving a mottled appearance. A very dark or black appearance can occur
- D: Diameter – if a mole is getting bigger it should be reviewed.
- E: Evolving – if a mole changes it should be reviewed
WHAT ARE THE STAGES OF MALIGNANT MELANOMA?
Pre-melanoma (lentigo maligna) and the earliest phase of melanoma (in-situ melanoma) are almost always cured with surgery. For melanoma beyond these early stages, it is the depth into the skin that the melanoma reaches that tells us how the disease might behave. This depth is termed the ’Breslow thickness’. The Breslow thickness will determine whether you require a simple excision or furthermore complex surgery including lymph gland biopsy.
The degree of spread a melanoma has undergone will be classified by stages:
- Stage I: Localised to the original site only
- Stage II: Localised to the skin only – the original site plus local skin spread
- Stage III: Spread to the nearby lymph glands
- Stage IV: Spread to the internal organs of the body
For more information on malignant melanoma, please see the British Association of Dermatologists website melanoma advice leaflets for stage 1, stage 2, stage 3, and stage 4 melanoma.
AM I MORE LIKELY TO GET MALIGNANT MELANOMA AGAIN IF I'VE HAD IT BEFORE?
If you have already had melanoma, there is a chance it may return again, particularly if the cancer was more advanced or widespread. Your doctors will discuss this with you and will regularly monitor you for signs it has returned.
skin cancer INSIGHTS AND ADVICE
When Should I Worry About A Mole
WHEN SHOULD I WORRY ABOUT A MOLE? A mole is a coloured spot on the skin which is made up of a cluster of cells known as melanocytes which are responsible for producing the pigment in your skin. Sometimes these melanocytes grow in a cluster
What are the common types of skin cancer?
WHAT ARE THE COMMON TYPES OF SKIN CANCER? There are three main types of skin cancer, basal cell carcinoma (BCC), squamous cell carcinoma (SCC) and melanoma. The first two are both known as non-melanoma skin cancer and are the most common varieties. Non-melanoma skin cancer

Skin Cancer Awareness Month
Skin cancer awareness month takes place every May with the aim of raising awareness of the dangers of unprotected sun exposure and educating on the ways skin cancer can be prevented. During skin cancer awareness month, the British Association of Dermatologists (BAD) also runs a